Understanding Scoliosis
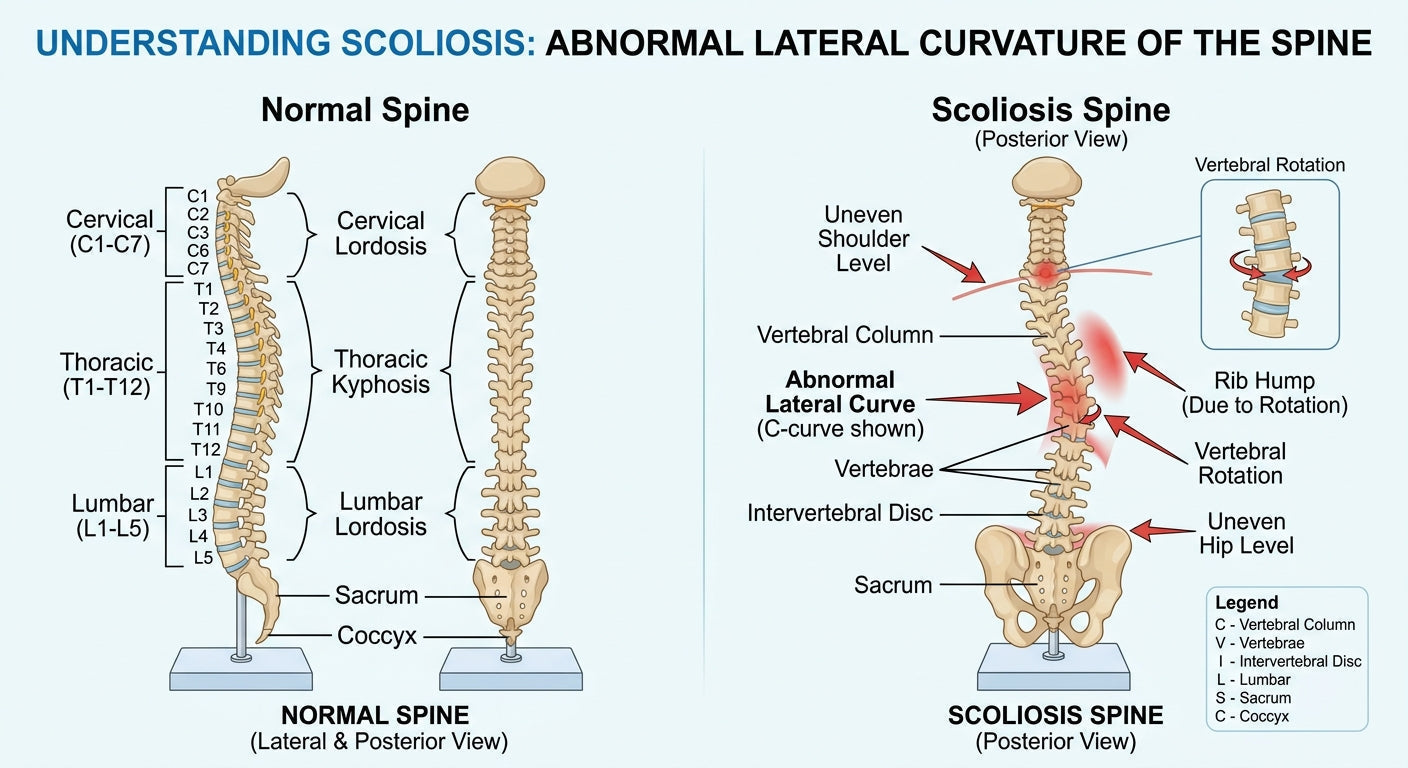
Scoliosis is a condition characterized by an abnormal sideways curvature of the spine, often resembling an "S" or "C" shape. While a slight curve might be harmless, significant scoliosis can cause pain, discomfort, and, in severe cases, affect lung and heart function. Affecting millions worldwide, scoliosis can manifest at any age, though it is most commonly diagnosed during adolescence. 
Understanding the Different Types of Scoliosis
Scoliosis isn't a single condition but rather a spectrum of spinal deformities, each with its unique characteristics and origins. Identifying the specific type of scoliosis is crucial for determining the most effective course of action.
-
Idiopathic Scoliosis: This is the most common form, accounting for about 80% of all cases. "Idiopathic" means the cause is unknown. It's often subdivided by the age of onset:
- Infantile Idiopathic Scoliosis: Diagnosed from birth to 3 years.
- Juvenile Idiopathic Scoliosis: Diagnosed from 4 to 10 years.
- Adolescent Idiopathic Scoliosis (AIS): Diagnosed from 10 to 18 years, this is the most prevalent type.
- Congenital Scoliosis: This type is present at birth due to abnormal development of the vertebrae during fetal growth. It can result from malformed vertebrae (such as wedge vertebrae or hemivertebrae) or vertebrae that fail to separate properly.
- Neuromuscular Scoliosis: This form develops due to underlying neurological or muscular conditions that affect the control of the spinal muscles. Common associated conditions include cerebral palsy, muscular dystrophy, spina bifida, and spinal cord injuries. Muscle weakness or imbalance leads to progressive curvature.
- Degenerative Scoliosis (Adult Onset): This type typically develops in adulthood, often after the age of 50. It's caused by the degeneration of discs and facet joints in the spine, leading to a loss of stability and a gradual sideways curve. This is sometimes referred to as adult de novo scoliosis.
- Syndromic Scoliosis: This form is associated with various syndromes or disorders, such as Marfan syndrome and Ehlers-Danlos syndrome, that affect connective tissue and can lead to spinal abnormalities.
Recognizing the Symptoms of Scoliosis
Early detection of scoliosis can significantly improve outcomes. While some cases are asymptomatic, common signs and symptoms include:
- Uneven shoulders, with one shoulder blade appearing more prominent.
- One hip appears higher than the other.
- Uneven waistline.
- Leaning to one side.
- A noticeable hump on one side of the back when bending forward (known as the Adam's forward bend test).
- Back pain, especially in adult scoliosis.
- Fatigue of the spine after prolonged sitting or standing.
- Difficulty breathing in severe cases, due to reduced chest space.
Diagnosis: How Scoliosis is Identified
The diagnostic process typically begins with a physical examination, during which a healthcare professional will look for the telltale signs mentioned above. The Adam's forward bend test is a key screening tool. If scoliosis is suspected, imaging tests are usually ordered:
- X-rays: Full-length X-rays of the spine are standard to confirm the presence of a curve, measure its angle (Cobb angle), and assess spinal maturity.
- MRI (Magnetic Resonance Imaging): May be used if neurological symptoms are present or if an unusual curve pattern suggests an underlying cause.
- CT Scan (Computed Tomography): Provides detailed bone imaging and may be used for surgical planning.
Treatment Options for Scoliosis
The approach to managing scoliosis is highly individualized, depending on the type, the severity of the curve, the patient's age, and the potential for progression.
Non-Surgical Management:
For milder curves, particularly in growing adolescents, observation is often the first step. Regular check-ups monitor the curve for progression.
- Physical Therapy and Exercises: Specific exercises, often part of a Schroth method or similar approach, can help strengthen core muscles, improve posture, and enhance spinal flexibility. While these won't correct a structural curve, they can help manage pain and improve function.
- Bracing: For growing adolescents with moderate curves (typically between 20 and 40 degrees Cobb angle) that are progressing, a spinal brace may be recommended. The goal of bracing is not to correct the existing curve but to prevent it from worsening until skeletal maturity. Modern braces are custom-fitted and designed to be worn for many hours a day. Discussions around can you wear a back brace to bed often arise, as consistent wear is vital for efficacy. Different types of support, such as lumbar support options, can be considered for general comfort, but specific scoliosis braces are tailored for curve management. Many individuals seek a posture support that helps maintain spinal alignment and improve posture. For conditions like spinal stenosis that sometimes accompany degenerative scoliosis, finding the right back brace for spinal stenosis is crucial for managing discomfort. For general aches, back pain support can offer much-needed relief and stability.
- Pain Management: Over-the-counter pain relievers, heat, ice, and gentle stretching can help alleviate discomfort. For persistent pain, a healthcare professional may recommend other interventions.
Surgical Intervention:
Surgery is typically reserved for severe curves (usually over 45-50 degrees Cobb angle in growing individuals) that are progressive and have not responded to non-surgical treatments, or for curves causing significant pain or impacting organ function. The most common surgical procedure is spinal fusion, where vertebrae are fused together using bone grafts and stabilized with rods and screws to correct the curvature and prevent further progression. The recovery period involves careful post-operative care, and questions about the back brace after surgery are common as patients seek to support their healing spine.
Living with Scoliosis
Managing scoliosis extends beyond clinical treatments to encompass daily lifestyle choices and emotional well-being.
- Stay Active: Regular, appropriate exercise can help maintain flexibility and strengthen muscles that support the spine. Consult a physical therapist for a tailored exercise program.
- Maintain Good Posture: Be mindful of your posture during daily activities, whether sitting, standing, or lifting. While a structural curve cannot be "corrected" by posture alone, good habits can minimize strain.
- Ergonomics: Ensure your workspace, bed, and common seating areas are ergonomically designed to support your spine.
- Emotional Support: Living with a chronic condition can be challenging. Seeking support from family, friends, support groups, or mental health professionals can be invaluable.
- Regular Monitoring: Continue regular check-ups with your healthcare provider to monitor your spine's condition and address any new symptoms.
For some, a back brace or posture corrector might be part of their daily routine for added support and awareness.
-
Veröffentlicht in
Back pain causes