Shoulder Arthroscopy
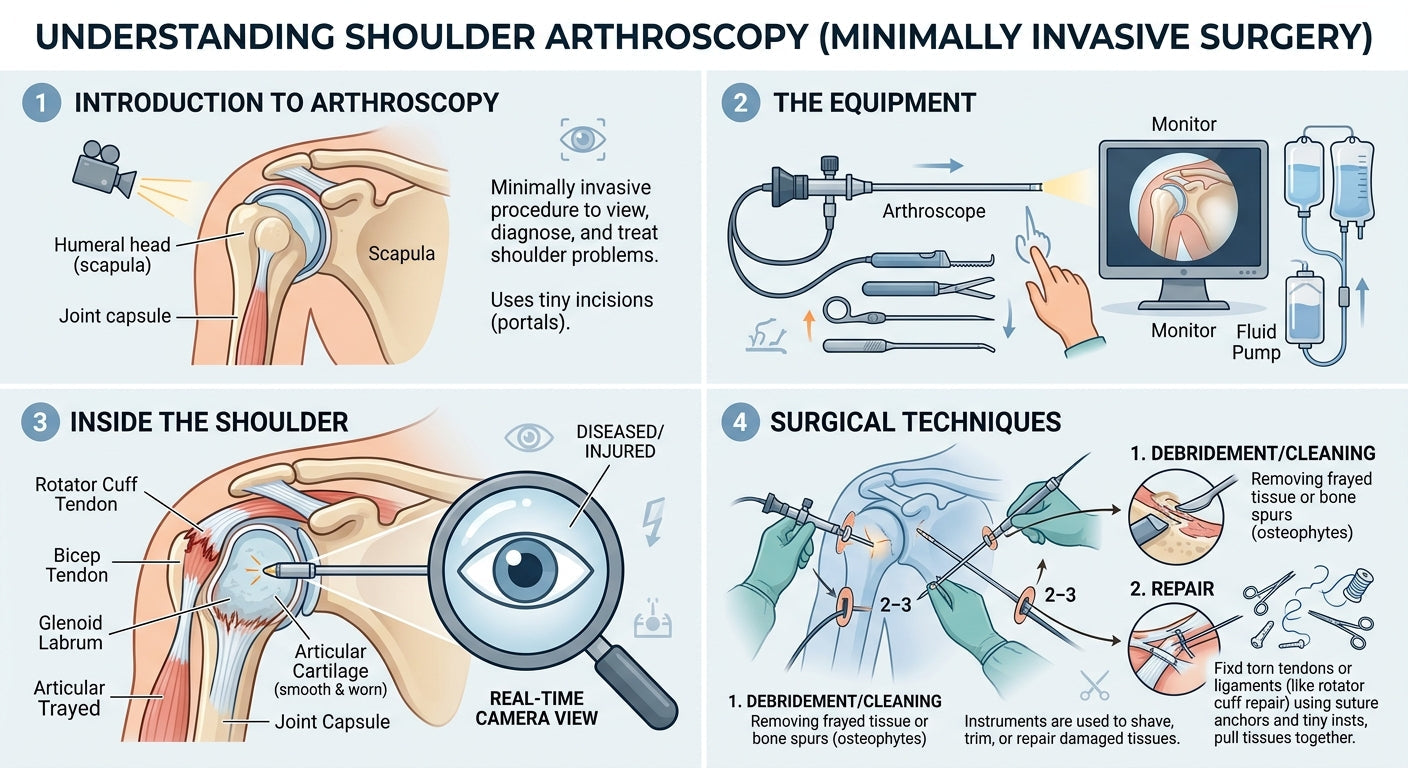
Shoulder arthroscopy is a sophisticated surgical technique that allows orthopedic specialists to diagnose and treat a wide range of shoulder problems with minimal invasiveness. Using small incisions, a miniature camera (arthroscope), and specialized instruments, this procedure provides a clear view of the joint without the need for large incisions. Patients often experience less pain, smaller scars, and a quicker return to daily activities compared to traditional open surgery.
When Is Shoulder Arthroscopy Recommended?
This minimally invasive procedure is typically considered when non-surgical treatments, such as physical therapy, rest, and medication, have not provided adequate relief. It's an effective option for various conditions affecting the shoulder joint.
Common reasons an orthopedic professional might recommend shoulder arthroscopy include:
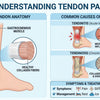
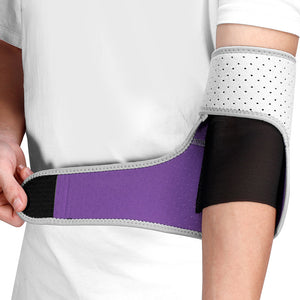
- Rotator Cuff Tears: Repairing torn tendons in the group of muscles and tendons surrounding the shoulder joint. Many wonder if a torn rotator cuff heal on its own, but often, significant tears require surgical intervention. Post-surgery, a shoulder brace for torn rotator cuff can provide essential support.
- Shoulder Impingement: Removing inflamed bursa or portions of bone that rub against the rotator cuff, causing pain and restricted movement. Wearing a shoulder impingement brace might be part of conservative or post-operative care.
- Labral Tears: Repairing tears in the labrum, the rim of cartilage around the shoulder socket, which can occur from trauma or repetitive motion.
- Shoulder Instability and Dislocations: Tightening stretched or torn ligaments that cause recurrent shoulder dislocations. A shoulder brace for dislocation can be crucial for stabilization and prevention. In some cases, a double compression shoulder brace may be considered for robust support.
- Inflammation: Removing inflamed joint lining (synovitis) or bursa (bursitis). Understanding the bursitis shoulder brace can help manage certain symptoms.
- Cartilage Damage: Repairing or smoothing damaged cartilage surfaces within the joint.
- Removal of Loose Bodies: Extracting fragments of bone or cartilage that can cause pain and catching sensations.
- Frozen Shoulder (Adhesive Capsulitis): Releasing stiff, scar tissue that restricts shoulder movement.
 Compare the key benefits, quantified risks, and a typical 3–6-month recovery timeline to decide whether shoulder arthroscopy fits your treatment goals.
Compare the key benefits, quantified risks, and a typical 3–6-month recovery timeline to decide whether shoulder arthroscopy fits your treatment goals.
Recovery and Rehabilitation
Recovery after shoulder arthroscopy is a crucial phase that significantly impacts the long-term success of the surgery. Most patients go home the same day.
- Immediate Post-Op: You'll likely experience some pain, which can be managed with prescribed pain relief. Regular icing of the shoulder helps reduce swelling and discomfort. The sling is essential for immobilizing the shoulder, protecting the repair, and facilitating initial healing.
- Physical Therapy: This is a cornerstone of recovery. A tailored physical therapy program will begin shortly after surgery, often starting with gentle range-of-motion exercises. As healing progresses, exercises will advance to improve flexibility and strength and, ultimately, restore full function to your shoulder.
- Timeline: The overall recovery timeline varies widely based on the specific procedure performed, your general health, and your commitment to rehabilitation. While some light activities might be resumed within weeks, a full return to strenuous activities or sports can take several months. It's common to wonder if shoulder braces work in speeding recovery, and while they offer support, consistent physical therapy remains key. Understanding how to heal a sprained shoulder involves similar principles of rest, gradual movement, and strengthening, which are echoed in post-surgical recovery. You might also need guidance on how to put on a shoulder brace correctly for optimal support during recovery.
-
Veröffentlicht in
Shoulder pain