Frozen Shoulder
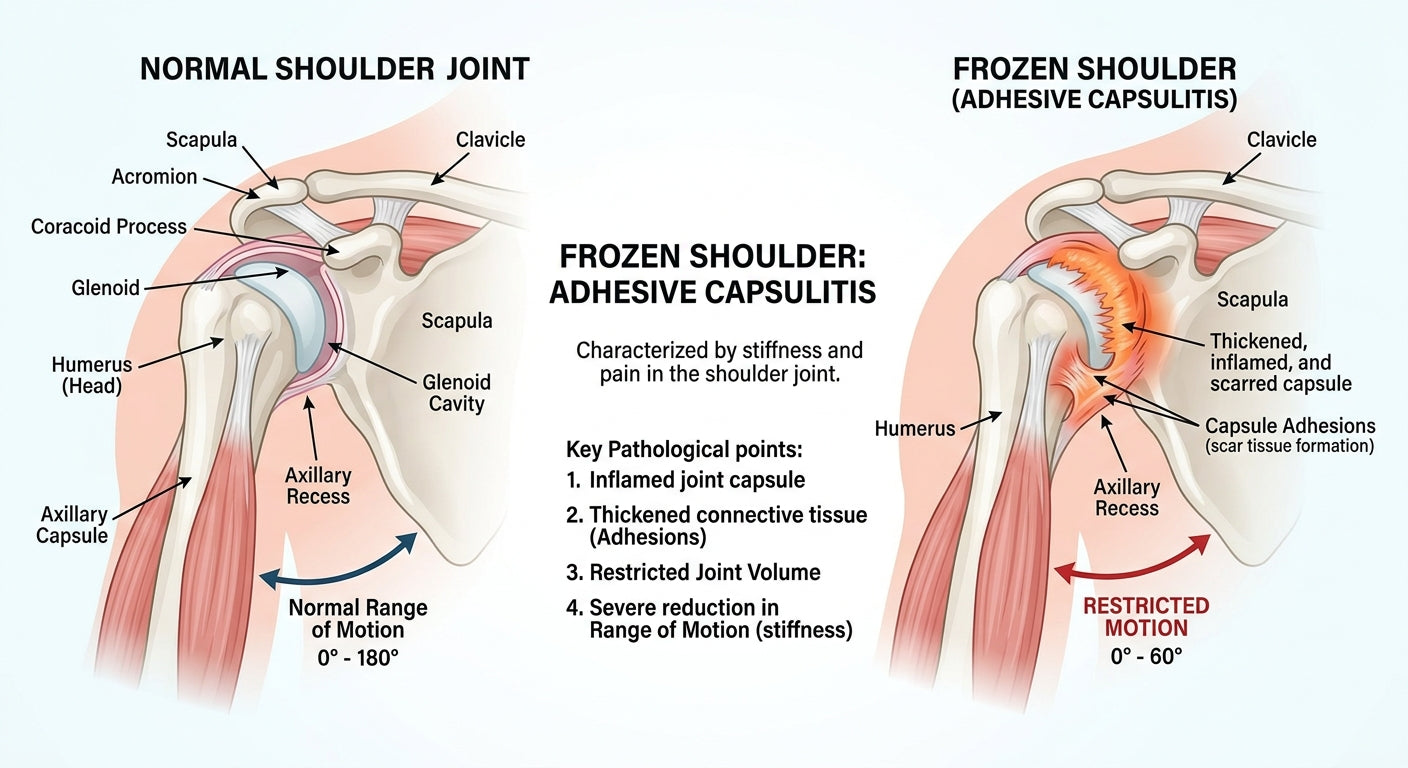
Frozen shoulder, medically known as adhesive capsulitis, is a condition characterized by stiffness and pain in the shoulder joint. It gradually restricts your range of motion, making everyday tasks challenging. While it is often painful and debilitating, understanding its nature, stages, and management options can empower individuals on their path to recovery.
What is Frozen Shoulder?
Frozen shoulder occurs when the capsule of connective tissue surrounding the shoulder joint thickens and tightens around the joint, restricting its movement. This capsule normally helps lubricate and protect the joint, allowing for smooth motion. However, in frozen shoulder, scar tissue forms within the capsule, causing it to become inflamed, stiff, and ultimately "frozen." The condition doesn't typically result from an injury, but rather develops slowly over time, often without a clear initiating event.
Stages of Frozen Shoulder
Frozen shoulder typically progresses through three distinct stages, each with its own set of symptoms and duration:
1. The Freezing (Painful) Stage
This initial stage is marked by a gradual onset of shoulder pain. As the pain worsens, the shoulder slowly loses range of motion. Activities like reaching overhead or behind your back become increasingly difficult. This stage can last anywhere from 6 weeks to 9 months.
2. The Frozen (Stiffening) Stage
During this stage, the pain may start to diminish, but the stiffness becomes more pronounced. Shoulder movement becomes significantly limited, sometimes to the point that even small movements are restricted. Despite the reduction in pain, the shoulder remains stiff, making daily activities very challenging. This stage typically lasts 4 to 12 months.
3. The Thawing (Recovery) Stage
This is the recovery phase where shoulder motion slowly begins to improve. The capsule gradually loosens, and the range of motion returns, often to near-normal. Pain continues to decrease. This stage can be the longest, lasting from 6 months to 2 years, or even longer in some cases.
Causes and Risk Factors
- Systemic Diseases: Conditions like diabetes, thyroid disorders (hypo- or hyperthyroidism), heart disease, and Parkinson's disease are strongly associated with an increased risk.
- Immobility: Prolonged shoulder immobility due to injury, surgery (such as a mastectomy or rotator cuff repair), or stroke can significantly increase the risk. Sometimes, seemingly minor incidents that lead to inactivity can trigger the condition. For a broader understanding of shoulder issues, it's helpful to be aware of common causes of shoulder injuries.
- Age and Gender: Frozen shoulder is most common in individuals aged 40 to 60 and is more prevalent in women.
- Previous Shoulder Trauma: While not a direct cause, prior shoulder injuries can sometimes precipitate shoulder immobility, which can lead to frozen shoulder.
Symptoms
The primary symptoms of frozen shoulder include:
- Dull or aching pain in the outer shoulder area, sometimes extending into the upper arm.
- Pain that worsens with movement and often at night, disturbing sleep.
- Gradual loss of shoulder motion, both active (when you try to move it yourself) and passive (when someone else tries to move it for you).
Diagnosis
Diagnosing frozen shoulder typically involves a thorough physical examination by a healthcare professional. They will assess your range of motion, both active and passive, and look for specific patterns of limited movement. Imaging tests like X-rays are often used to rule out other conditions such as arthritis or bone spurs. In some cases, an MRI may be ordered to visualize the soft tissues and confirm joint capsule thickening.
After the introduction, before the treatment details
Treatment and Management
The good news is that frozen shoulder often improves on its own, though it can take considerable time. The goal of treatment is to control pain and restore motion.
Conservative Treatment
- Pain Management: Over-the-counter pain relievers such as NSAIDs (nonsteroidal anti-inflammatory drugs) can help reduce pain and inflammation. In some cases, prescription medications may be necessary. Applying heat or cold packs can also provide temporary relief.
- Physical Therapy: This is a cornerstone of recovery. A physical therapist will guide you through stretching and range-of-motion exercises designed to loosen the stiff joint and improve flexibility. Consistency with a home exercise program is crucial.
- Corticosteroid Injections: Injections of corticosteroids directly into the shoulder joint can help reduce pain and inflammation, especially during the painful freezing stage, allowing for more effective physical therapy.
- Hydrodilatation: This procedure involves injecting a large volume of sterile fluid into the joint capsule to stretch and break up adhesions.
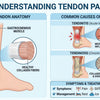
While some patients wonder if shoulder braces work for frozen shoulder, their role is typically limited. They may offer comfort and support during daily activities, but they don't directly "thaw" the shoulder. However, for those with other shoulder concerns, various shoulder braces are available. If you're considering using a shoulder compression brace for comfort, consult with your healthcare provider or physical therapist. It's also worth noting that the effectiveness of a shoulder brace good for tendonitis or a rotator cuff brace help shoulder restore normal function differs significantly from what is needed for frozen shoulder. People often ask whether a shoulder brace can heal a rotator cuff, but frozen shoulder management is distinct.
Recovery and Prognosis
Recovery from frozen shoulder requires patience and persistent effort. It's a long process, often taking 1 to 3 years from onset to full recovery. Adhering to your physical therapy program and continuing exercises at home is vital for regaining a full range of motion. While most people recover completely, some may experience residual stiffness or minor limitations in motion.
Prevention
While primary frozen shoulder can be challenging to prevent, especially when underlying health conditions are present, certain strategies can reduce the risk of secondary frozen shoulder:
- Early Mobilization: After a shoulder injury or surgery, it's crucial to begin gentle range-of-motion exercises as advised by your healthcare professional.
- Manage Underlying Conditions: Effectively managing conditions such as diabetes or thyroid disorders can help mitigate risk.
-
Posted in
Shoulder pain