Can Sciatica Cause Knee Pain?

The relationship between back discomfort, leg symptoms, and seemingly localized joint issues like knee pain can be complex and often misunderstood. While the knee joint itself is a common source of localized pain, a significant proportion of lower extremity complaints can be traced back to the spine. For clinicians and patients alike, understanding the intricate neural and biomechanical pathways connecting the lumbar spine to the knee is crucial for accurate assessment and management. This article explores the compelling mechanisms by which sciatica, an irritation of the longest nerve in the body, can manifest as or contribute to knee pain.
What is Sciatica?
Sciatica is not a diagnosis but rather a general term describing symptoms caused by irritation or compression of the sciatic nerve or the spinal nerve roots that form it. These nerve roots originate in the lower (lumbar) spine, specifically from L4 through S3. The nerve itself travels deep within the buttock, down the back of the thigh, where it divides above the knee into the tibial and common peroneal nerves, and continues down to the foot.
The characteristic symptom of sciatica is pain that radiates along this nerve pathway. This pain can vary widely, ranging from a dull ache to a sharp, burning sensation or electric shock-like feeling. It is often accompanied by numbness, tingling (paresthesia), or muscle weakness in the affected leg. The primary cause is typically a disc herniation, spinal stenosis, piriformis syndrome, or a lumbar spine degenerative condition that directly impinges upon one of the contributing nerve roots. Although symptoms most commonly affect the buttocks and the back of the thigh, the nerve’s extensive reach into the lower leg means that symptoms can sometimes present in unexpected regions, including the area around the knee.
Overview of Common Causes of Knee Pain
To correctly attribute knee pain to sciatica, it is essential to first consider the more common, local origins of knee discomfort. The knee joint, being the largest and one of the most mechanically stressed joints in the body, is susceptible to a wide array of local pathologies. The most frequent causes of knee pain include:
- Osteoarthritis (OA): Degenerative joint disease, leading to the breakdown of cartilage and subsequent bone-on-bone friction, causing deep, activity-related pain.
- Patellofemoral Pain Syndrome (PFPS): Often referred to as "runner's knee," this involves pain around or under the kneecap, typically exacerbated by activities like climbing stairs, squatting, or prolonged sitting.
- Ligamentous Injuries: Trauma, such as tears to the anterior cruciate ligament (ACL), medial collateral ligament (MCL), or posterior cruciate ligament (PCL), is often associated with acute instability and swelling.
- Tendonitis/Tendinopathy: Inflammation or degeneration of tendons, such as the patellar tendon (jumper's knee) or the quadriceps tendon.
- Meniscal Tears: Damage to the cartilage shock absorbers within the joint, resulting in pain, clicking, or locking sensations.
These local conditions are generally diagnosed through specific physical tests, imaging (like X-rays or MRI), and the patient's history of localized trauma or specific mechanical symptoms. When these localized sources have been ruled out, or when the knee pain presents with associated neurological symptoms, the focus must shift superiorly to the lumbar spine and the sciatic nerve pathway.
Sciatica-Associated Knee Pain: Underlying Pathophysiological Links
The question of whether sciatica can cause knee pain is answered affirmatively through a trifecta of interconnected mechanisms: direct neural transmission, altered movement patterns, and joint stress compensation.
- Nerve Impingement and Referred Pain
The most direct link is through the phenomenon of referred pain. The spinal nerve roots that contribute to the sciatic nerve carry sensory information from various structures, including the skin, muscles, and joints of the lower limb. Specifically, the L4 and L5 nerve roots, common sites of sciatic irritation, supply sensation to the skin around the knee and the structures within the joint capsule.
When a nerve root is compressed or inflamed in the lumbar spine (e.g., by a herniated disc), the brain interprets the pain signal as originating from the entire territory supplied by that nerve, not just the site of compression. This can lead to the sensation of pain being perceived in the knee area, even though the primary pathology is in the lower back. This referred pain is distinct from actual knee damage; it is purely a neurological signal misinterpretation. The pain is often described as vague, deep, or burning and may not correlate with specific knee movements. Furthermore, the L5 nerve root provides motor innervation to muscles like the tibialis anterior, and S1 to the gastrocnemius. Irritation can lead to weakness or cramping that alters the biomechanical load on the knee.

- Muscular Imbalance and Compensation
Mechanics Sciatic nerve irritation often leads to weakness or inhibition of the muscles it innervates, particularly the hamstrings, gluteals, and calf muscles. This inhibition forces other muscles in the kinetic chain to compensate, profoundly affecting the knee joint's alignment and stability.
For instance, if the gluteus medius muscle (innervated by the superior gluteal nerve, which is closely linked to the same spinal segments as the sciatic nerve) is inhibited, the pelvis can drop on the unsupported side during walking (Trendelenburg sign). This leads to an increased adduction and internal rotation of the femur, dramatically altering the tracking of the patella and increasing stress on the medial compartment of the knee. Over time, this chronic muscular compensation can contribute to conditions like patellofemoral pain syndrome or accelerate degenerative changes, essentially creating a secondary knee problem that was initiated by the sciatic nerve pathology. This is a critical factor when assessing the long-term efficacy of a knee brace for sciatic pain—if the underlying issue is muscular compensation due to sciatica, addressing the spine is paramount.
- The Joint Chain Reaction
The human lower limb functions as a kinetic chain, where movement or pathology at one joint influences all others. The chain reaction often starts at the pelvis and hip, which is the site of the nerve root impingement. Sciatica-related pain and muscle guarding in the hip and gluteal region lead to restricted hip rotation and extension.
To maintain a normal gait (walking pattern), the body must find the missing range of motion elsewhere. This compensatory motion is often sourced from the knee, causing the knee to excessively rotate or extend during the stance and swing phases of gait. For example, a stiff hip due to pain might force a "corkscrew" motion at the knee. The chronic, abnormal loading and torsion placed on the knee joint structures (ligaments, menisci, and cartilage) that are not designed for this compensatory rotation can ultimately lead to microtrauma and inflammatory responses, resulting in objective knee pain and sometimes swelling. Addressing the lumbar spine and hip mobility is often necessary to break this joint chain reaction. The use of a hip brace may sometimes be considered to stabilize the pelvis and reduce aberrant motion, but this must be integrated with a comprehensive spinal treatment plan.
Identifying When Knee Pain May Originate from Sciatica
Differentiating between local knee pathology and referred pain from sciatica requires a systematic approach based on symptoms and physical signs. Key indicators suggesting a sciatic origin include:
- Associated Back/Buttock Pain: The knee pain is almost always accompanied or preceded by low back pain or pain/tingling in the buttock or posterior thigh.
- Neurological Signs: The presence of numbness, tingling, or demonstrable muscle weakness in the entire lower leg (not just localized to the knee).
- Movement Patterns: The knee pain is often worse with activities that increase nerve root tension, such as specific positions of the spine (e.g., sitting for long periods, bending forward) or the straight leg raise test. Local knee pain, by contrast, is usually aggravated by weight-bearing activities or specific joint angles (e.g., deep squatting).
- Vague Distribution: The pain is typically diffuse, poorly localized around the knee, and may track down the back of the calf or into the foot.
- Absence of Local Trauma: No history of direct injury, twisting, or impact to the knee joint itself.
When these systemic, neurological, and positional components are present, it strongly suggests that the symptoms being experienced at the knee are a referred or secondary mechanical effect of a primary sciatic nerve irritation.
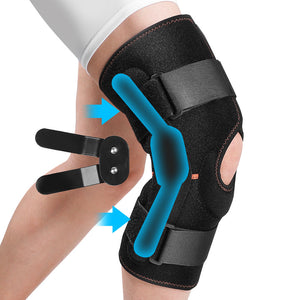
Support and Bracing: Protecting the Knee and Supporting the Overall Chain
While bracing is a common intervention for localized knee instability or pain (as addressed by a knee brace for pain), the role of bracing changes when the underlying cause is sciatic nerve irritation or compensatory mechanics. In this context, the aim shifts from purely supporting the knee to stabilizing the entire kinetic chain and managing nerve-related symptoms.
Traditional knee braces can offer temporary symptomatic relief by providing compression, warmth, and proprioceptive feedback. However, they do not resolve the upstream mechanical fault. In some cases, a Fivali knee brace for sciatica nerve pain might be utilized to manage the biomechanical effects of sciatica-induced weakness, such as an ankle-foot orthosis (AFO) if foot drop is present, which secondarily helps stabilize the knee during gait.
In the case of sciatica, attention often turns to the hip and lower back. Bracing options in this area include:
- Lumbar Supports/Corsets: Used to limit excessive movement in the lower spine, which can help unload an irritated disc or facet joint, potentially calming the nerve root.
- Sacroiliac (SI) Belts: Applied to stabilize the pelvis if the sciatica is linked to SI joint dysfunction, aiming to normalize the foundational movement base of the entire leg.
Questions such as do sciatic nerve leg braces work must be viewed with caution. There is no singular brace that "cures" sciatica. The effectiveness of any support device is entirely dependent on its integration into a comprehensive treatment plan that addresses the specific nerve root compression or irritation. Supportive devices are palliative tools for stabilizing segments or managing symptoms, not definitive treatments for the underlying nerve pathology.
Products You May Be Interested In:
< >Professional Intervention and Lifestyle Recommendations
Managing knee pain that stems from sciatica requires a multi-faceted approach focused on decompressing and calming the irritated nerve, improving spinal and hip mobility, and correcting the compensatory movement patterns that stress the knee. Intervention strategies often include:
- Manual Therapy: Techniques applied to the spine, hip, and pelvis to restore joint mobility, reduce muscle tension, and improve nerve glide.
- Targeted Exercise: A specific exercise program is vital. This typically includes exercises for:
- Spinal Stabilization: Strengthening the core musculature (transversus abdominis, multifidus) to provide a stable base and reduce shear forces on the lumbar discs.
- Gluteal Strengthening: Re-activating and strengthening the gluteal muscles (maximus and medius) to correct pelvic stability and reduce compensatory hip/knee rotation.
- Nerve Gliding (Neurodynamics): Specific exercises designed to gently move the sciatic nerve within its sheath, improving its tolerance to movement and reducing sensitivity.
- Modalities: The judicious use of heat, ice, or transcutaneous electrical nerve stimulation (TENS) can assist in managing acute pain and muscle guarding along the nerve pathway.
Lifestyle adjustments play a key role in long-term management. These include: maintaining an active lifestyle that incorporates regular, low-impact exercise (like swimming or cycling); paying attention to proper lifting techniques to minimize lumbar spine strain; optimizing workspace ergonomics, especially for prolonged sitting; and maintaining a healthy body weight to reduce overall load on the spine and joints. Consistency in applying these preventative measures can significantly reduce the likelihood of sciatic flare-ups and the subsequent development of secondary knee issues.
Conclusion
The connection between the lumbar spine and the knee is undeniable. While the knee is frequently the site of pain, the origin of that pain may be found hundreds of millimeters away in the lower back. Sciatica can lead to knee pain through direct nerve signal misinterpretation (referred pain) and, perhaps more significantly, through creating chronic muscular imbalances and joint chain reactions that cause secondary damage to the knee structures. Differentiating between local pathology and nerve-mediated pain requires a careful assessment that considers the entire kinetic chain. Successful management relies on identifying and treating the root cause—the irritated sciatic nerve—while employing support and rehabilitation strategies to protect the distal joint structures from the effects of compensation.