Thumb Arthritis
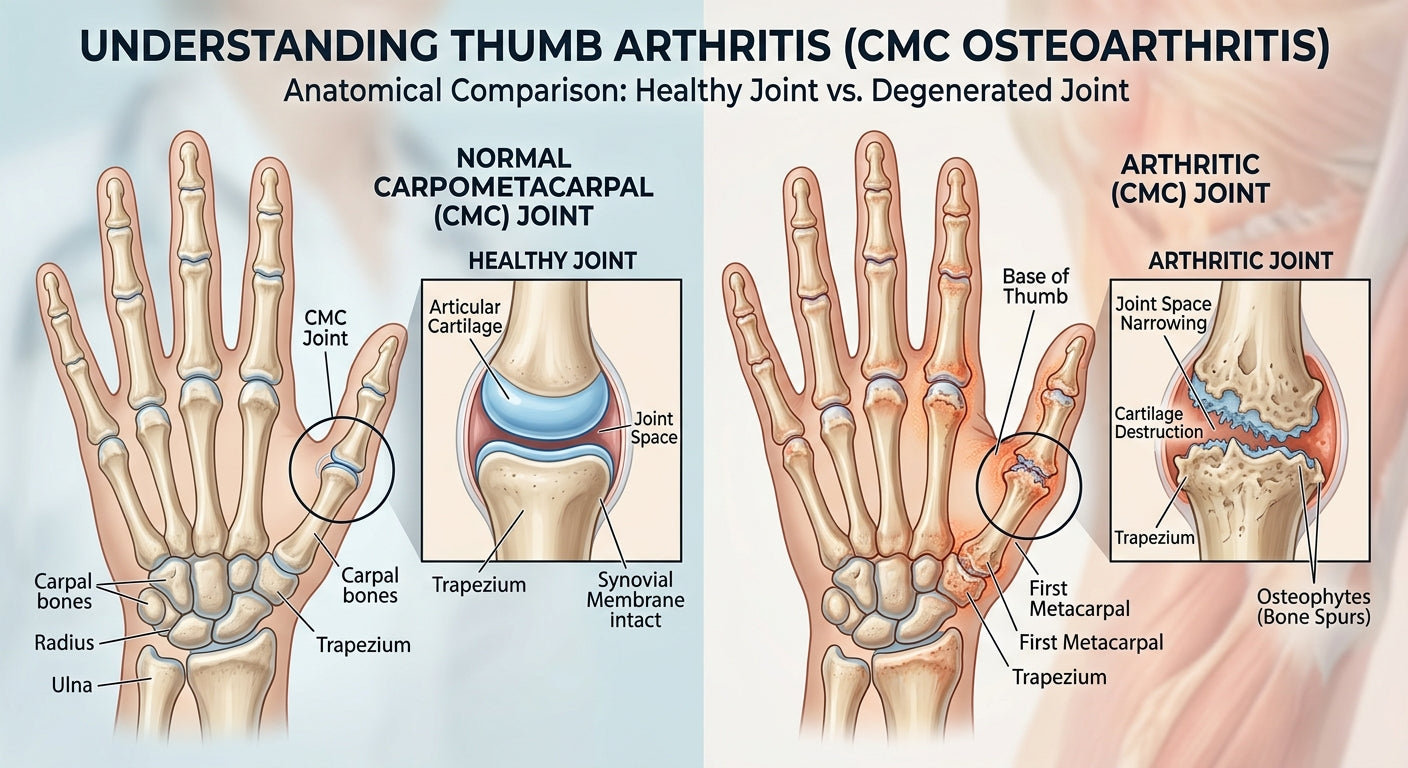
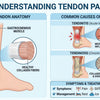
Thumb arthritis, medically known as basal joint arthritis or carpometacarpal (CMC) joint arthritis, is a common condition that affects the joint at the base of your thumb. This crucial joint allows a wide range of motion, essential for gripping, pinching, and twisting. When the cartilage cushioning the ends of the bones in this joint wears away, it can cause pain, stiffness, and loss of strength in the thumb, significantly affecting daily activities.
While thumb arthritis can develop at any age, it is most common in individuals over 40 and is significantly more prevalent in women than in men.
What Causes Thumb Arthritis?
The primary cause of thumb arthritis is the degeneration of the articular cartilage in the CMC joint. This cartilage provides a smooth, gliding surface for the bones, but over time, it can thin and become rough. This wear and tear leads to bones rubbing directly against each other, causing inflammation, pain, and eventually, bone spurs.
Several factors can contribute to the development or progression of thumb arthritis:
- Age: The risk increases with age as cartilage naturally wears down.
- Gender: Women are more susceptible, possibly due to hormonal factors or differences in joint anatomy and laxity.
- Genetics: A family history of thumb arthritis can increase your likelihood of developing it.
- Prior Injury: Previous fractures, dislocations, or other trauma to the thumb joint can predispose it to early arthritis.
- Repetitive Stress: Activities that involve repetitive gripping, pinching, or twisting of the thumb, such as certain occupations or hobbies, can contribute to wear and tear.
- Other Conditions: Inflammatory forms of arthritis, such as rheumatoid arthritis, can also affect the CMC joint, though typical thumb arthritis is often osteoarthritis.
Recognizing the Symptoms of Thumb Arthritis
- Pain at the base of the thumb: This is often the most prominent symptom and can range from a dull ache to sharp, intense pain, especially during activities that involve pinching, grasping, or twisting. You might also wonder, "Why does my thumb hurt when I press on it?"
- Stiffness: The thumb joint may feel stiff, particularly in the morning or after periods of inactivity.
- Swelling: Visible swelling at the base of the thumb may result from inflammation.
- Tenderness: The joint may be tender to the touch.
- Decreased Strength: Pinching or gripping objects may become difficult and feel weak.
- Limited Range of Motion: It may become challenging to fully move the thumb, which can affect tasks such as opening jars or turning keys.
- Deformity: In advanced stages, the joint may appear enlarged or "square" at the base of the thumb, and a bony bump may develop.
- Grinding Sensation: You might experience a grinding, clicking, or popping sensation when moving the thumb joint.
Diagnosing Thumb Arthritis
A healthcare professional will typically diagnose thumb arthritis based on a physical examination and a review of your symptoms and medical history. During the examination, they will assess the range of motion, stability, and tenderness of your thumb joint. X-rays are often used to confirm the diagnosis, show the extent of cartilage loss, and reveal any bone spurs or other joint damage.
Once diagnosed, your healthcare provider will discuss various treatment approaches tailored to your specific condition and lifestyle.
 Quickly compare expected pain relief, strength gains, and recovery time between conservative care and surgical options for thumb arthritis to make an informed treatment choice.
Quickly compare expected pain relief, strength gains, and recovery time between conservative care and surgical options for thumb arthritis to make an informed treatment choice.
Treatment Options for Thumb Arthritis
Treatment for thumb arthritis generally begins with conservative, non-surgical methods and progresses to surgical intervention if symptoms persist or worsen.
Conservative Management (Non-Surgical)
- Rest and Activity Modification: Avoiding activities that aggravate the thumb, such as repetitive pinching or heavy gripping, can help reduce pain and inflammation. Modifying how you perform tasks can also make a significant difference.
- Cold/Heat Therapy: Applying ice packs can help reduce swelling and pain, while heat can soothe stiff joints.
- Supportive Devices: Wearing a thumb support or splint can stabilize the joint, limit motion, and provide rest, thereby reducing pain. There are various designs, from simple wrist thumb support to more comprehensive options such as spica splints or thumb guard braces. These supports can be especially helpful during activities or while sleeping. For general joint stabilization, individuals often look for products like the ones offered by Fivali. When dealing with discomfort, some might find a wrist brace for pain beneficial if the pain radiates.
-
Medication:
- Over-the-counter pain relievers: Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen can help manage pain and inflammation.
- Topical medications: Creams or gels containing NSAIDs can be applied directly to the affected joint.
- Prescription medications: Stronger NSAIDs or other pain relievers may be prescribed by your doctor.
- Physical and Occupational Therapy: A therapist can teach you exercises to improve the range of motion, strength, and stability in your thumb. They can also provide guidance on joint protection techniques and ergonomic adjustments to reduce stress on the joint during daily activities. Learning how to wrap a sprained thumb or even how to tape sprained thumb can also provide temporary relief and support. For conditions like bone-on-bone arthritis, even if affecting other joints, these principles of support and pain management are crucial. These often come from a wider variety of wrist and thumb supports.
Injections
If conservative treatments don't provide sufficient relief, your doctor might recommend injections into the joint.
- Corticosteroid Injections: These powerful anti-inflammatory medications can provide temporary pain relief and reduce swelling. However, their effects are not permanent, and repeated injections are typically limited due to potential side effects.
- Hyaluronic Acid Injections: Also known as viscosupplementation, these injections aim to replenish the joint's natural lubricating fluid, potentially reducing pain and improving function.
Surgical Options
Common surgical approaches include:
- Trapeziectomy: This is the most common surgery for thumb arthritis, involving the removal of the trapezium bone (one of the small bones at the base of the thumb). A tendon may be used to create a new cushion or stabilize the joint.
- Fusion (Arthrodesis): This procedure permanently fuses the bones of the CMC joint, eliminating pain but also all movement at that joint. It is typically reserved for severe cases where stability is paramount.
- Arthroplasty (Joint Replacement): In some cases, the damaged joint may be replaced with an artificial joint (prosthesis). This aims to relieve pain while preserving motion.
Living with Thumb Arthritis
- Ergonomic Tools: Use tools with large, easy-to-grip handles to reduce stress on your thumb joint.
- Regular Exercise: Maintain overall fitness and hand strength through gentle exercises recommended by a therapist.
- Weight Management: If you are overweight, losing excess weight can indirectly reduce stress on all joints, including the thumb.
- Stay Informed: Work closely with your healthcare team to understand your condition and treatment options.
Thumb arthritis can be a challenging condition, but with proper diagnosis and a tailored management plan, you can effectively alleviate pain, improve hand function, and continue to engage in your daily activities.
-
Posted in
Wrist Injury