Pelvic Pain
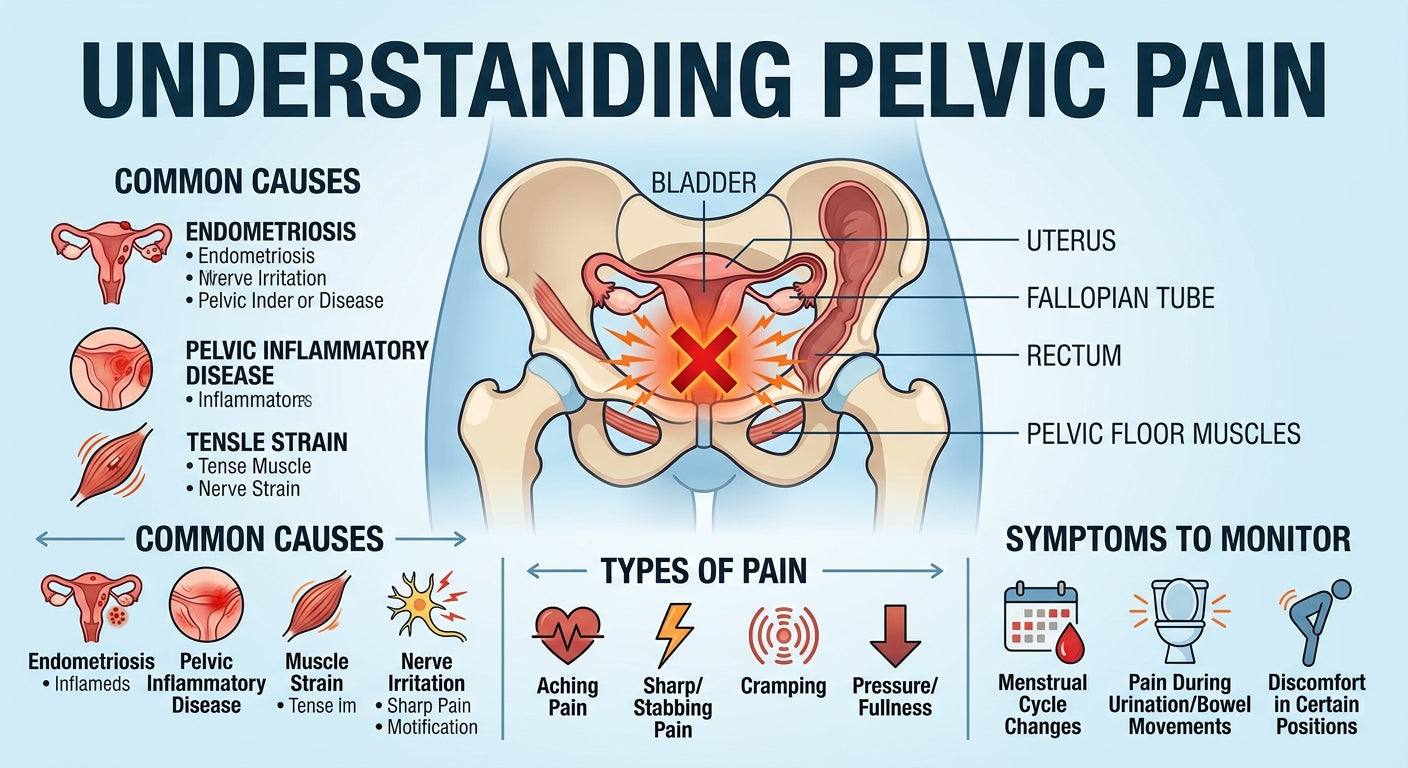
Pelvic pain is a common and often debilitating condition affecting millions of individuals, primarily women, but it can also impact men. It refers to pain felt in the lower abdomen and pelvis, below the belly button, and between the hips. This discomfort can be acute (sudden and severe) or chronic (lasting six months or more), and its impact ranges from mild annoyance to severe interference with daily life.
Understanding the Scope of Pelvic Pain
Pelvic pain can originate from various organs and systems within the pelvic region, including the reproductive, urinary, and digestive tracts, as well as the musculoskeletal and nervous systems. Because of its complex origins, diagnosing the exact cause can be challenging and may require a thorough medical evaluation.

Causes of Pelvic Pain
-
Gynecological Causes (in women):
- Endometriosis: A condition where tissue similar to the lining of the uterus grows outside the uterus.
- Adenomyosis: Endometrial tissue grows into the muscular wall of the uterus.
- Uterine Fibroids: Non-cancerous growths of the uterus.
- Ovarian Cysts: Fluid-filled sacs that develop on the ovaries.
- Pelvic Inflammatory Disease (PID): An infection of the female reproductive organs, often a complication of sexually transmitted infections.
- Ectopic Pregnancy: When a fertilized egg implants outside the uterus.
- Ovulation Pain (Mittelschmerz): Mid-cycle pain associated with egg release.
- Menstrual Cramps (Dysmenorrhea): Severe pain during menstruation.
-
Urological Causes:
- Urinary Tract Infections (UTIs): Infections in any part of the urinary system.
- Interstitial Cystitis (Painful Bladder Syndrome): Chronic bladder pain with no known cause.
- Kidney Stones: Hard deposits of minerals and salts that form inside the kidneys.
-
Gastrointestinal Causes:
- Irritable Bowel Syndrome (IBS): A common disorder affecting the large intestine, causing cramping, abdominal pain, bloating, gas, and diarrhea or constipation.
- Crohn's Disease and Ulcerative Colitis (Inflammatory Bowel Diseases): Chronic inflammation of the digestive tract.
- Diverticulitis: Inflammation or infection of small pouches (diverticula) that can form in the intestines.
- Constipation: Infrequent or difficult bowel movements.
-
Musculoskeletal Causes:
- Pelvic Floor Dysfunction: Tightness, weakness, or spasms of the pelvic floor muscles.
- Fibromyalgia: A chronic disorder characterized by widespread pain, tenderness, and fatigue.
- Hernias: When an organ or fatty tissue squeezes through a weak spot in a surrounding muscle or connective tissue.
- Sciatica: Pain radiating along the sciatic nerve, which runs down one or both legs from the lower back. This can manifest as sciatica support issues and contribute to pelvic discomfort. Individuals looking for relief from sciatic hip pain may find valuable information on how to address this specific concern.
-
Nerve-Related Causes:
- Nerve Entrapment: When a nerve becomes compressed or irritated.
-
Psychological Factors:
- Stress, anxiety, and depression can exacerbate or contribute to chronic pain experiences.
Recognizing Symptoms of Pelvic Pain
- Dull aches or sharp, stabbing pains.
- Constant pain or intermittent spasms.
- Pain during urination or bowel movements.
- Discomfort during sexual intercourse (dyspareunia).
- Pain that worsens with prolonged standing or certain movements.
- Radiating pain to the lower back, hips, or legs.
- Feeling of pressure or heaviness in the pelvis.
- Fatigue and difficulty sleeping due to pain.
Keeping a pain journal can help individuals and their healthcare providers identify patterns and potential triggers.
Diagnosing Pelvic Pain
- Medical History: A detailed discussion about the pain, its characteristics, duration, any related symptoms, and medical background.
- Physical Examination: This may include a general physical exam, abdominal exam, and a pelvic exam for women, or a rectal exam for men and women, to assess tenderness, masses, or other abnormalities.
-
Imaging Tests:
- Ultrasound: Uses sound waves to create images of pelvic organs.
- CT Scan (Computed Tomography): Provides detailed cross-sectional images.
- MRI (Magnetic Resonance Imaging): Offers highly detailed images of soft tissues.
- Laboratory Tests: Blood and urine tests can check for infection, inflammation, or pregnancy.
- Laparoscopy: A minimally invasive surgical procedure where a small incision is made to insert a thin, lighted scope to view the pelvic organs directly. This is often used to diagnose conditions like endometriosis.
Treatment and Management Strategies
-
Medications:
- Pain Relievers: Over-the-counter options like NSAIDs (ibuprofen, naproxen) or prescription pain relievers.
- Hormonal Therapies: For gynecological conditions, hormonal birth control or GnRH agonists can manage pain related to menstrual cycles or endometriosis.
- Antibiotics: If an infection is present.
- Muscle Relaxants: To ease pelvic floor muscle spasms.
- Antidepressants/Nerve Pain Medications: Sometimes used at lower doses to manage chronic pain by affecting pain pathways.
-
Physical Therapy:
- Pelvic Floor Physical Therapy: Involves exercises, manual therapy, and biofeedback to strengthen, relax, or re-coordinate pelvic floor muscles. This can be particularly effective for muscle-related pain and certain types of sciatica. Guidance on back support for sciatica can often complement physical therapy approaches, especially when considering comprehensive pain management.
- General Physical Therapy: To address posture, gait, and overall body mechanics that might contribute to pelvic pain.
-
Lifestyle Adjustments and Complementary Therapies:
- Heat Therapy: Applying heat packs can soothe muscle tension.
- Stress Management: Techniques like mindfulness, meditation, and yoga can help manage the emotional impact of chronic pain.
- Dietary Changes: For gastrointestinal conditions like IBS, dietary modifications can significantly reduce symptoms.
- Acupuncture: Some individuals find relief through traditional Chinese medicine.
-
Injections and Procedures:
- Nerve Blocks: Injections to numb specific nerves contributing to pain.
- Trigger Point Injections: To relieve pain in tight muscle knots.
- Surgical Interventions: In cases where conservative treatments are ineffective or for specific conditions like severe endometriosis, fibroids, or adhesions. Surgery may involve removing problematic tissue or, in rare cases, a hysterectomy. When considering various treatment paths, it's beneficial to understand how different support systems can aid recovery and ongoing management. For those experiencing hip discomfort, exploring various hip support solutions can provide much-needed relief. Additionally, when assessing options for nerve-related pain, it’s helpful to investigate exploring hip support for sciatica, which can be a key component in a broader pain management plan. Patients may also benefit from understanding targeted compression for hip and sciatic support to alleviate discomfort in specific areas. Further, understanding how to permanently address sciatica can empower patients with the knowledge to develop long-term strategies.
When to Seek Medical Attention
It is important to consult a healthcare provider if you experience:
- Severe or sudden pelvic pain.
- Pelvic pain that worsens over time or interferes with daily activities.
- Pain accompanied by fever, chills, nausea, vomiting, or unexplained weight loss.
- Pain during sexual intercourse or urination.
Early diagnosis and intervention are key to effective management of pelvic pain. A healthcare professional can help pinpoint the cause and develop a personalized treatment plan to help you find relief.
-
Posted in
Hip Injury