Shoulder Bursitis
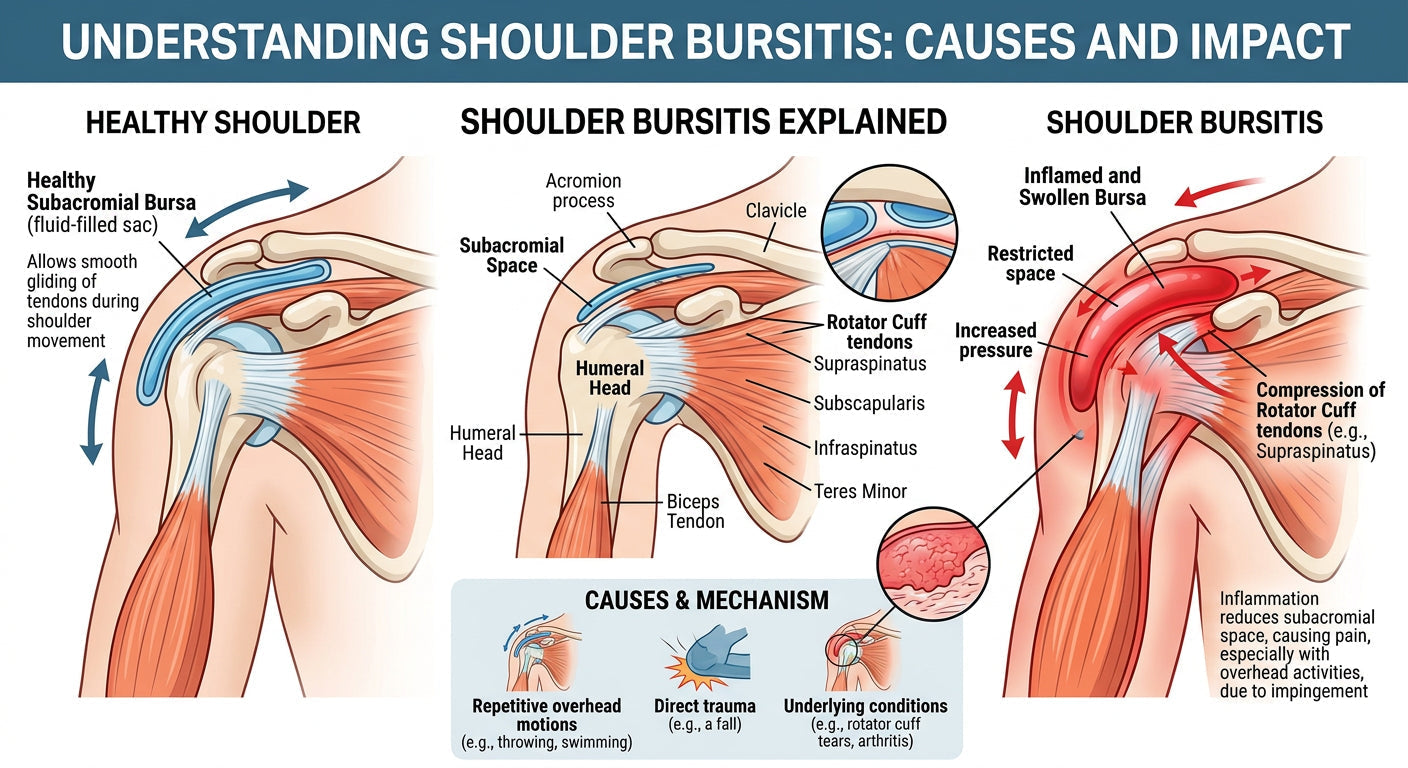
Shoulder bursitis is a common condition characterized by inflammation of the bursa, a small, fluid-filled sac that reduces friction between bones, tendons, and muscles around the shoulder joint. When these protective sacs become irritated or inflamed, it can cause significant pain and limit the shoulder's range of motion, affecting daily activities and overall quality of life.
What is Shoulder Bursitis?
The shoulder joint contains several bursae, with the subacromial bursa being the most frequently affected in cases of bursitis. This bursa sits between the rotator cuff tendons and the acromion (part of the shoulder blade). Its role is to allow smooth gliding during arm movements, particularly when raising the arm overhead.
When this bursa becomes inflamed—a condition known as shoulder bursitis—its lining thickens and produces excess fluid, causing it to swell. This swelling then compresses the surrounding structures, including the sensitive rotator cuff tendons, leading to pain, tenderness, and restricted movement. While often associated with overuse, bursitis can also stem from other underlying issues.
Common Causes of Shoulder Bursitis
- Repetitive Overhead Activities: Sports like swimming, tennis, and baseball, as well as activities like painting, gardening, or lifting objects overhead, can irritate the bursa over time.
- Direct Trauma: A direct blow or fall onto the shoulder can cause acute bursitis.
- Poor Posture: Sustained poor posture can alter shoulder mechanics, increasing friction and bursal irritation.
- Muscle Imbalance and Weakness: Weakness in the rotator cuff muscles or the surrounding shoulder stabilizers can lead to improper shoulder movement, increasing strain on the bursa.
- Other Shoulder Conditions: Bursitis often co-occurs with other shoulder issues, such as shoulder tendonitis, rotator cuff injuries, or impingement syndrome. For instance, sometimes a shoulder brace for a torn rotator cuff might be considered if these conditions are present simultaneously.
- Systemic Conditions: Certain inflammatory conditions, like rheumatoid arthritis, gout, or diabetes, can increase the risk of developing bursitis. To learn more about the common causes of shoulder injuries in general, you can explore further resources.
Recognizing the Symptoms
The symptoms of shoulder bursitis can vary in intensity but typically include:
- Pain: A dull ache or sharp pain in the outer part of the shoulder, often radiating down the arm. The location of the pain in the bursa sac can sometimes indicate which bursa is affected.
- Pain with Movement: Worsening pain when raising the arm out to the side or overhead, reaching behind the back, or sleeping on the affected side.
- Tenderness: The shoulder may be tender to the touch, especially on the top or outer aspect.
- Stiffness: A feeling of stiffness and limited range of motion in the shoulder joint.
- Swelling and Redness: While less common, visible swelling or redness around the shoulder can occur in more severe cases.
Diagnosis of Shoulder Bursitis
- Medical History: Discussing your symptoms, activities, and any past injuries.
- Physical Examination: Assessing your shoulder's range of motion, strength, and tenderness. Specific tests can help differentiate bursitis from other conditions like rotator cuff tears or tendonitis.
-
Imaging Tests:
- X-rays: Primarily used to rule out bone spurs, arthritis, or other bony abnormalities.
- Ultrasound: Can visualize the bursa directly, showing inflammation and fluid accumulation. It can also assess the rotator cuff tendons.
- MRI: Provides detailed images of soft tissues, useful for confirming bursitis and identifying coexisting conditions such as tendon tears.
Treatment and Recovery
The treatment for shoulder bursitis primarily focuses on reducing pain and inflammation, restoring shoulder function, and preventing recurrence. The approach often begins with conservative methods, escalating to more advanced interventions if necessary.

Conservative Treatment Options
- Rest: Avoid activities that aggravate the shoulder. This doesn't mean complete immobilization, but rather modifying activities to prevent further irritation.
- Ice: Applying ice packs to the affected area for 15-20 minutes several times a day can help reduce pain and swelling.
- Over-the-Counter Pain Relievers: Non-steroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen can help manage pain and inflammation.
-
Physical Therapy: A physical therapist can design a program of exercises to:
- Improve range of motion.
- Strengthen the rotator cuff and surrounding shoulder muscles.
- Correct muscle imbalances.
- Improve posture and movement, mechanics.
- Activity Modification: Learning proper techniques for lifting, carrying, and performing daily tasks can prevent re-injury.
- Supportive Devices: Sometimes, a shoulder brace for bursitis can provide gentle compression and support, helping limit irritating movements and allowing the bursa to heal. For issues like rotator cuff injuries, understanding how a shoulder brace can help restore normal function can be beneficial.
Recovery and Prevention
The recovery time for shoulder bursitis varies depending on the severity and adherence to treatment. Mild cases may improve within a few weeks, while more chronic or severe conditions might take several months. Understanding how long bursitis typically lasts can help manage expectations.
To prevent recurrence:
- Warm-up and Stretch: Always warm up before physical activity and perform appropriate stretches.
- Gradual Increase in Activity: Avoid sudden increases in the intensity or duration of activities that stress the shoulder.
- Ergonomics: Ensure your workspace and daily activities are ergonomically sound to minimize shoulder strain.
- Strengthen Shoulder Muscles: Maintain strength and flexibility in the shoulder and rotator cuff muscles through regular exercise.
- Listen to Your Body: Pay attention to pain signals and rest or modify activities as needed.
-
Posted in
Shoulder pain